Check your motions on the Bristol Stool Chart
The Bristol Stool Chart is a pictorial examination of the type of stools you are passing.
Aunt Vadge: post-antibiotic fissures – what can I do?
Antibiotics trigger a yeast infection that ends in drying and fissures. Find out how to fix it.
Pain and bleeding after fingering – is it normal?
A young lady bleeds after being fingered by a boy she likes. Find out why.
Vaginal fissures
Learn how to treat and manage vaginal cuts, abrasions, tears and other wounds from sex, fingering, accidents, and disease. Dry skin, cuts, and abrasions can cause pain and soreness, so learn how to help them heal faster.
What to do if you lose your tampon
Safe tips on how to get your lost tampon out, even if it's sideways!
Candida albicans vaginal yeast infections
Candida albicans is one cause of a yeast infection.
My Vagina’s repository
Articles about bacterial vaginosis, aerobic vaginitis (AV), yeast infections and more
Choosing the best lubricant for the job
Choosing the right lube for the job is important, to keep yourself, your partner, and your toys safe. Learn what you can and can't use as a lube during sex play.
Female sexuality
Female sexuality is a complex and worthwhile topic to explore, which has had far too little airtime in the past few hundred years.
Dairy-free milk kefir ferments
You can also make milk kefir with soy, coconut and almond milk, but you must give it some time in cow's milk every few weeks.
What are milk kefir grains?
A rundown of what milk kefir grains are and how we use them to help support a healthy vaginal microbiome.
How to take care of your milk kefir
Learn how to take care of your milk kefir grains and get the most out of them every day. Clear instructions and FAQs.
Perineoplasty
The perineoplasty procedure is used to either tighten, loosen or cosmetically augment the perineal area between the anus and the vaginal opening.
Vulvodynia
Vulvodynia is a vulvar pain condition that may have its roots in several different areas, with treatments varying between cases.
Medicines that affect your libido
Some medications will have a negative impact on your sexual appetites, arousal, and ability to orgasm.
How tampons work
Tampons are convenient, but they can also have unwanted effects on your vagina.
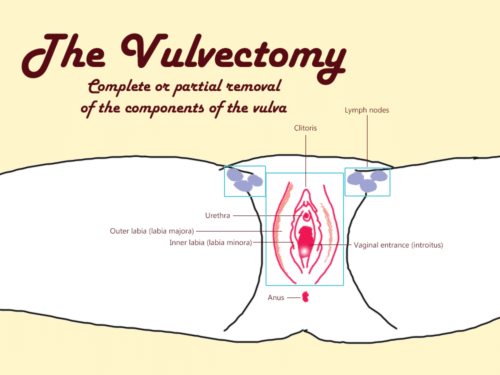
The vulvectomy
Vulvectomy is the surgical removal of all or parts of the vulva, as part of treating a disease that has not responded to other treatments. A vulvectomy is a serious operation where the inner and outer labia, clitoris, and lymph nodes of the groin are removed.
Understanding and managing painful sex (dyspareunia)
Dyspareunia is the medical term for painful sex, however this pain may have a variety of causes. Painful penetration can occur at the entrance to the vagina, or deep inside, or both.
Understanding and treating pelvic inflammatory disease (PID)
Discover the causes, symptoms, and treatments of PID, and why it can be hard to treat. We offer effective some non-drug teatment options.
Understanding and treating vulvodynia
Vulvodynia is a vulvar pain condition with a variety of causes, and thus a variety of treatments.