A simple vaginal or vulvar tear means a cut, split or damage to tissue that may bleed a little, sting when you urinate and feel uncomfortable.
A cut may be from mysterious causes or it could be from something you know you did (scratches, sex wounds, etc.).
The Simple Tear
If your cut or tear was caused by an identifiable action (sex, tampons, fingering, toys, fiddling) and stings, bleeds and is uncomfortable, it will very likely heal by itself in a few days to a week. You can apply some vulvar-specific cuts cream to support healing.
How long it takes to heal will depend on how deep the vulvar or vaginal cut is. The deeper the cut, the longer it will take to heal.
Take a look in a hand mirror or take a photo with your phone so you know what to expect based on how deep the vulvar cut or tear is.
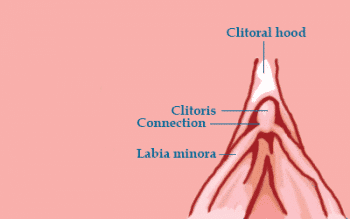
The joins between the clitoral hood and labia (see diagram) and the posterior fourchette are all prone to being split or cut, even sometimes from the slightest pull in the wrong direction.
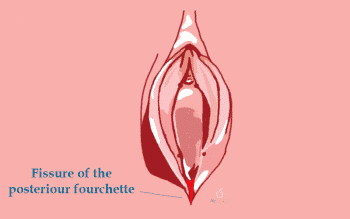
Recurrent fissuring of the posterior fourchette
The posterior fourchette is one of the most common places where a vagina or vulva can tear. The posterior fourchette is the very bottom of the V-shape created by the bottom of the vaginal entrance (the introitus).
Because penetration with fingers, a toy or a penis can easily result in a tear in this area, recurrent fissuring of the posterior fourchette is a common complaint amongst those who are sexually active.
The posterior fourchette is the first place to split when pressure is applied since it is where the two halves of our body join when we’re growing in the womb. It’s the weakest spot when you consider the other pressure spots of penetration.
No other place will split the same way or anywhere near as easily. If repeated damage is done to the posterior fourchette, scar tissue may form, making the vaginal entrance even smaller.
This scarring may require some repair strategies, but a full investigation should be undertaken to determine if scarring is an issue.
If you have repeated posterior fourchette fissuring, see your doctor or gynaecologist for advice.
How to care for vulvar and vaginal cuts and tears
Vaginal skin heals very quickly, just like the mouth, so prevent further damage by avoiding irritation
- Use some vulvar-specific cream to support healing
- No sex, tampons, masturbating, lacy underwear
- Keep it clean with daily showering or a rinse
- Go commando (no underwear) or wear comfortable underwear so the healing cut doesn’t catch or irritate your skin
- Keep an eye on it, protect it, keep it clean, and don’t fret about it
- Posterior fourchette fissures (the fork in the bottom of the vaginal entrance) can start to branch into the realm of the Deep and Nasty Tear which you need to seek advice for and treat differently
Rough sex or fingering
Vaginal tears, bleeding and pain after fingering are really common in sexually inexperienced people who just aren’t sure what’s supposed to be happening to their vagina.
While it comes naturally to a chosen few, fingering is advanced sex and takes a lot of practice to get right for most of us.
See our Fingering Basics article for instructions for lovers on how to use fingers for pleasure without causing bleeding and pain.
Navigating (gentler) sex
Additionally, sex should not leave you with wounds, so be gentle, communicate with your partner about what feels good and what doesn’t (even if it’s awkward – practice makes it less so), and make use of a good-quality lubricant.
Sex should never (unless you are being deliberately kinky) result in pain and bleeding.
If you are getting sex wounds, perhaps it’s time to revisit Sex 101 or seek treatments for any medical condition (like lichenoid conditions) that may be causing skin to easily split.
Vaginal tear caused by tampons
During your period, heavy or incorrect use of tampons can cause splits in the entrance to your vagina.
This type of sore usually occurs when changing a tampon when the previous one isn’t completely full (still a bit dry), then putting another one in straight away.
These cuts or sores can also happen when you are inserting tampons incorrectly.
See our section on tampons if you are struggling to get it right.
Vaginal fissures should resolve quickly once your period is over, but it is important to learn how to correctly insert a tampon. Tampons are not supposed to cause damage.
Yanking a tampon out – don’t do it!
Additionally, yanking a tampon out like pulling a band-aid off can cause internal damage to the lining of your vagina. Don’t do it!
Wait until the tampon has absorbed moisture over a couple of hours, and then slowly pull it out using the string.
If you are concerned, see your local sexual health clinic or emergency room. They can quickly help you with a vulvar or vaginal cut.
What a health professional can do for your cuts and tears
The medical way of dealing with vaginal cuts and tears – outside of those that require surgical or other medical intervention – is, like naturopathy, to let them heal by themselves.
Your doctor’s approach
Your doctor will see what’s wrong and provide you with a diagnosis for your vaginal tear. Depending on the diagnosis, some examples of what your doctor may prescribe for a vulvar or vaginal cut include:
- Antibiotic cream, gel or tablets to prevent or treat an infection
- Anti-fungal cream or tablets for a yeast infection
- Antivirals for herpes to reduce a flare-up
- Oestrogen cream for atrophic vaginitis (dry, irritated vaginal tissue)
- Topical steroids for dermatitis, psoriasis or lichenoid disorders to reduce inflammation
- Topical anaesthetic for pain
Your naturopath’s approach
Your naturopath may offer you the same treatments, but in a herbal cream (like our vulva and vagina-friendly cuts cream) or another formula depending on your diagnosis.
Either way, your cuts should heal up quickly without scarring. If they don’t, please see your healthcare professional for advice.
References
Kennedy CM, Manion E, Galask RP, Benda J. Histopathology of recurrent mechanical fissure of the fourchette. Int J Gynaecol Obstet. 2009;104(3):246–247. doi:10.1016/j.ijgo.2008.10.017
Belinda M Welsh, Karen N Berzins, Kathy A Cook and Christopher K Fairley Management of common vulval conditions. Med J Aust 2003; 178 (8): 391-395. || doi: 10.5694/j.1326-5377.2003.tb05257.x
Mac Bride MB, Rhodes DJ, Shuster LT. Vulvovaginal atrophy. Mayo Clin Proc. 2010;85(1):87–94. doi:10.4065/mcp.2009.0413
David A. Eschenbach, Soe Soe Thwin, Dorothy L. Patton, Thomas M. Hooton, Ann E. Stapleton, Kathy Agnew, Carol Winter, Amalia Meier, Walter E. Stamm, Influence of the Normal Menstrual Cycle on Vaginal Tissue, Discharge, and Microflora, Clinical Infectious Diseases, Volume 30, Issue 6, June 2000, Pages 901–907, https://doi.org/10.1086/313818
Carr PL, Felsenstein D, Friedman RH. Evaluation and management of vaginitis. J Gen Intern Med. 1998;13(5):335–346. doi:10.1046/j.1525-1497.1998.00101.x







